`
Author: hbuijs
How Drama Students Help Train Doctors
(From the UW College of Arts and Science, written by Nancy Joseph 5/2/2025 – https://artsci.washington.edu/news/2025-05/how-drama-students-help-train-doctors)
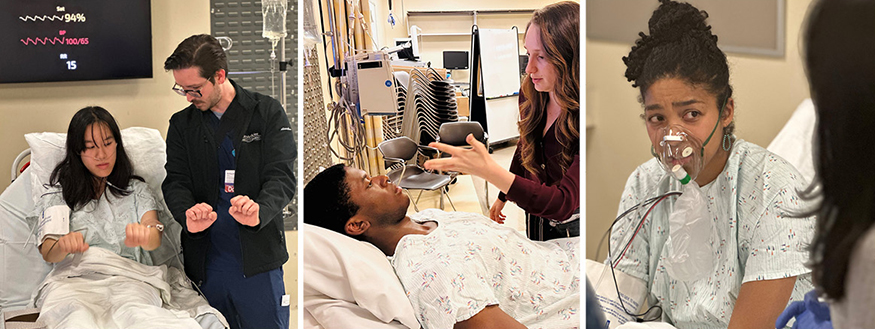
At Harborview Medical Center in Seattle, a patient lies on a gurney in a hospital gown. While answering questions posed by two UW Medicine neurology residents, the patient’s breathing grows labored and the residents must respond.
Across the hall, a 40-something mother and her adult daughter meet with another neurology resident to discuss the mother’s memory decline. While the daughter expresses concern, the mother makes light of recent memory lapses, chalking them up to depression, for which she is being treated.
Such scenarios are familiar for neurologists, but on this day they are simulations, with students from the UW College of Arts & Sciences’ School of Drama performing the roles of patients and family members. Through simulations, medical residents can hone their diagnostic and communication skills before they face similar scenarios with actual patients. The drama students benefit as well.
“I’ve wanted to act for a while, and I’ve always been interested in medicine, so this was a perfect combination,” says UW creative writing major and drama minor Lev Parker, who played the role of the patient on the gurney. “This was my first performance, my first stage.”
The Value of Simulations
Simulations are not new in health care — the UW has a “standardized patient” program involving simulations for clinical training — but neurology training has traditionally been “lecture-based with a lot of self study,” explains Wolfgang Muhlhofer, associate professor and vice chair of education in the UW Department of Neurology. “That’s not really putting our trainees’ active problem-solving, medical decision-making, and communication skills to work.”
“Simulations are really important because they rehearse for real life. …They allow us to engage and activate our whole bodies, our emotions, to gain knowledge and skills.”
Scott MagelssenProfessor, UW School of Drama
To address this, Neurology introduced a full-day “bootcamp” of simulation training for incoming residents in 2022. For the role of patients, Muhlhofer looked into using paid “standardized patients” through the UW’s standardized patient program, but the cost and lack of availability on the date of the planned bootcamp were barriers. So he reached out to School of Drama faculty about recruiting student actors as volunteers.
Initially, Drama faculty felt uncomfortable asking students to take on an acting job without payment. Then Scott Magelssen, professor of theater history and performance studies, offered to create a two-credit course for those interested in participating. Having spent his career studying simulations in various contexts — from living history museums to simulations preparing soldiers for combat — Magelssen knew how valuable simulations can be.

“Simulations are really important because they rehearse for real life,” Magelssen says. “They use the tools from theater and performance to create a world that is realistic enough that the training feels authentic. They allow us to engage and activate our whole bodies, our emotions, to gain knowledge and skills.”
Drama students signed up for Magelssen’s course and participated in the neurology boot-camp simulations. The simulations were so well received by neurology residents that Neurology began offering optional two-hour simulation workshops each quarter. Drama students have continued to be involved.
“I think our drama students are hungry for these kinds of experiences,” Magelssen says. “This was a way to have them participate in the simulations but also have an educational component, an opportunity to reflect on the ways they are using their skills and how their art can make an impact in the world outside of the theater.”
Preparing for the Unexpected
Like any acting role, the simulation actors arrive prepared, with guidance from Muhlhofer. He first sends an email describing upcoming simulation scenarios, then discusses the scenarios in more detail with interested students over Zoom. Before the event, the students get a script — “more like Cliff Notes,” Muhlhofer says — with information about their character and the story to tell the trainee physicians. The notes include things they should mention to the trainees, as well as things they shouldn’t volunteer and subtext for the character.
“Subtext is important because patients don’t just show up with a symptom,” says Muhlhofer. “They all have a story that they carry around with them. A lot of times I leave it up to the actors to improvise based on some basic personality traits, some basic emotions they should have in this particular situation.”
Muhlhofer meets with the actors in person for a dry run before the simulation event. He plays the role of the trainee physician and provides suggestions for making the patient’s physical symptoms and emotional responses as believable as possible. The more real the scenario feels, the more the neurology residents will learn from it, he explains.
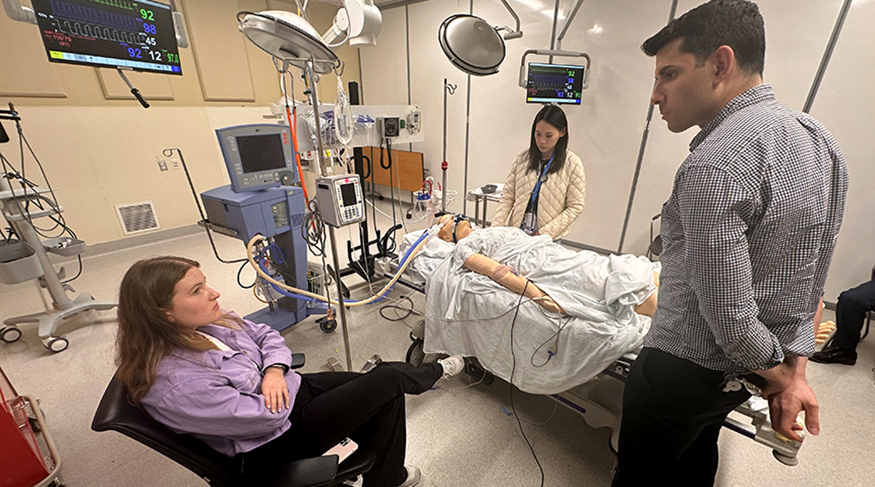
Sometimes Muhlhofer is surprised at how intense the experience can be for the residents. He recalls one scenario in which the patient complained of a headache and suddenly became unresponsive and had a seizure. “The calm scenario turned into this really high stress situation,” says Muhlhofer. “The resident was rushing around the bed, trying to interact with the patient. The resident’s pager fell to the ground, so the resident kicked it across the room to get it out of the way while yelling orders to the nurse. They had a visceral response to what was happening and got so into it that it felt real.”
Not all simulations are that dramatic, but there are always surprises — even for the actors. Colleen Carey, a comparative history of ideas major and drama minor, recalls playing the role of a patient admitted to the emergency room with a cluster of symptoms. The simulation was run twice with different trainees. Both sought the patient’s consent for immediate intubation, but one was somewhat brusque in delivering this difficult news while the other was skilled and empathetic. Each elicited a different response from Carey.
“Both simulations were not at all what I expected, and yet both offered surprising gifts about the art of medicine as well as the art of communication,” Carey says.
Though the simulations are designed for training neurologists, they also strengthen the drama students’ skills in building a character and improvising under pressure. “In their reflective essays, a lot of our students talk about how this experience helped them build their confidence as a performer,” Magelssen says. “Asked if they would recommend this experience to others, across the board they say ‘yes.’”
Some students, like Carey, have participated many times. With each simulation, she gains something new.
“I continue to find such profound purpose in this work,” Carey says. “There are lessons I continue to learn in this arena that cannot be learned anywhere else.”
Interested in participating in Department of Neurology simulations during the next academic year? Email Wolfgang Muhlhofer (Department of Neurology) at wmuhlho@uw.edu or Scott Magelssen (School of Drama) at mmagelss@uw.edu to learn more.
Shared Pain, Shared Healing: Headache Care Visits
Click the link below to read the UW Medicine Huddle that focus on our Headache Clinic, along with Dr Murinova.
Comprehensive, Research-driven Brain Tumor Care Supported by Neuropsychologists, Social Workers and Cancer Nutritionists

For the past 20 years, UW Medicine has been a leader in brain tumor care. Our faculty members provide advanced therapies to treat more than 100 kinds of brain tumors. Today, our leadership extends further as we are involved in multiple research efforts to improve the comfort level and extend survival for many patients.
“Patients with brain tumors have very special needs. Their tumors can strike at the heart of who they are as people, producing symptoms that affect language, memory and motor or sensory functioning,” says Lynne P. Taylor, MD, FAAN, FANA, the neuro-oncology co-director at the Alvord Brain Tumor Center at University of Washington Medical Center – Montlake. “As neuro-oncologists, we are working with our colleagues nationally to develop clinical trials to try and improve quality of life and overall survival.”
Taking research to the next level
The brain tumor team is currently involved in three clinical investigations that could open the door to better therapies in the future.
- Vaccines: As part of immunotherapy research, our investigators participate in a randomized-controlled clinical trial to examine whether the therapeutic vaccine SurVaxM can lengthen survival for patients with glioblastoma. Participants will receive one of two treatments: an oral pill: temozolomide (standard of care chemotherapy) with SurVaxM in Montanide (a milky solution to encourage the patient’s immune response) or temozolomide and saline in Montanide (placebo).
“In this trial, we’re attempting to use immunotherapy to stimulate the patient’s immune system to shut down tumor growth using survivin, a molecule that plays a large role in tumor aggressiveness and resistance to therapy,” she says.
- Drug combination therapy: In the GBM AGILE (Glioblastoma Adaptive Global Innovative Learning Environment) clinical trial, our researchers work with international partners to test multiple drugs and drug combinations to effectively combat glioblastoma.
“By participating in the GBM AGILE trial, we are contributing to a trial model that promotes rapid testing of multiple drugs and screening drug combinations to, hopefully, get us closer to finding an active agent against glioblastoma.”
- Targeted brain tumor therapy: Through the INDIGO clinical trial, our investigators helped confirm that the drug vorasidenib successfully targets the common IDH mutation in lower-grade primary brain tumors in younger patients.
“This is the first example of a targeted therapy of this kind having activity against primary brain tumors,” she says. “These types of tumors primarily occur in patients between the ages 20 and 45, and we may one day be able to delay treating them with chemotherapy or radiation therapy for several years. This delay is extremely important for people during the years in which they are interested in starting families and who, naturally, want to avoid toxic therapies that may impact fertility.”
Slowing and preventing brain tumors

The team focuses on improving the quality of life for the patients they see in their clinical practices. Through collaborations, our neurological surgeons, radiation oncologist and neuro-oncologists provide medical management for a wide variety of brain tumors both at the Alvord Brain Tumor Center and Fred Hutchinson Cancer Center, an independent organization that serves as UW Medicine’s cancer program. Together, we provide access to the latest the latest research, treatment options and clinical trials.
“We are also very lucky to have the support of neuropsychologists, social workers, cancer nutritionists and nurses specialized in the care of brain tumor patients. We treat symptoms of nervous system problems from a neurological perspective, but we also use chemotherapy and immunotherapy from an oncologic perspective,” Taylor says. “Our goals are to prevent other tumors from forming and to slow down the growth of any tumors surgeons cannot completely remove.”
Neurofibromatosis Clinic
- We are an NF-certified clinic through the Children’s Tumor Network. In the Neurofibromatosis Clinic, our experts treat people who have the genetic disorders neurofibromatosis types 1 and 2 and schwannomatosis. These can produce skull base tumors which can cause deafness. Some patients with schwannomas and meningiomas also benefit from bevacizumab, a monoclonal antibody that targets vascular endothelial growth factor (VEGF) expressed in abnormal tumor blood vessels, shrinking the tumors and preventing further hearing loss.
Gamma Knife Center and Proton Center
- Our radiation oncologists and neurological surgeons work closely together to deliver stereotactic radiosurgery (Gamma Knife) to patients with metastatic brain tumors to prevent future tumor growth.
- Proton radiation therapy is used for younger patients with lower grade brain tumors to limit the exit dose and preserve cognitive function in the future.
A comprehensive approach
To ensure our patients consistently receive the highest level of care, Taylor says our team takes a comprehensive approach to disease management through the dedicated Neuro-oncology Tumor Board.
Every week, they gather as a multidisciplinary group to discuss patient cases and decide on courses of care. In addition to neuro-oncologists and neurological surgeons, this team includes radiation oncologists, medical oncologists, neuropathologists, neuroradiologists, nurses and social workers.
Ultimately, Taylor says, it’s these partnerships that make us a sought-after institution for high-quality neurological care for patients with cancer.
Epilepsy Care: Collaborating to Prevent Seizures
Whether a patient receives a new diagnosis of epilepsy or they have struggled for years to manage their seizures, they need high-quality care from the partnership of their primary care provider and specialist. UW Medicine neurological surgeons and neurologists are trained to deliver the most advanced epilepsy therapies and treatments, offering relief for a condition that affects approximately 3 million people in the U.S.
“The brain is the coolest organ in the body, and epilepsy is a disorder of the brain’s electricity,” says UW Medicine neurologist Nicholas Pete Poolos, MD, PhD. “Epilepsy is one of our more treatable conditions.”
UW Medicine’s Regional Epilepsy Center is at the forefront of care, helping patients with this condition. Through close collaborations, our expert team of neurologists and neurological surgeons identifies and delivers the best treatments for each patient. We’re also leading the way with groundbreaking epilepsy research.
The importance of treating epilepsy
Every patient’s experience with epilepsy is different. Some people have one seizure a year, while others can suffer multiple episodes daily. Many individuals benefit from medications that can prevent seizures, but one-third of patients don’t respond to them, says Poolos, who directs the Regional Epilepsy Center. If patients don’t achieve seizure freedom after trying two to four medications, it’s unlikely they will find the right drug combination for seizure relief.
When epilepsy medications fail, surgical intervention to limit or eliminate seizures is critical, says UW Medicine neurological surgeon Andrew L. Ko, MD. If left uncontrolled, seizures can cause sudden unexpected death in epilepsy (SUDEP). In fact, over time, a patient’s SUDEP risk can equal the mortality risk for a patient with an aneurysm.
Ultimately, addressing a patient’s epilepsy and preventing seizures helps them return to their regular activities in a safe, healthy way.
“Treating epilepsy is about improving quality of life,” Ko says.“If you can make someone seizure-free, they can drive, sleep better, go back to work and have a better life.”
Delivering high-quality seizure care
Getting patients as close to seizure-free as possible is our top priority. Together, our team of nine neurologists, two board-certified neurological surgeons and two neurology nurse practitioners is uniquely positioned to help patients on this journey.
“We have the best-trained providers who can take on the hardest problems,” Poolos says. “We see the entire range of epilepsy patients. People come to us after their first seizure or when they’ve had epilepsy for years and are heading toward surgery after many medications failed.”
As a referral center, we serve a large patient volume from the Washington, Wyoming, Alaska, Montana and Idaho (WWAMI) region. According to Poolos, on average, our providers schedule 4,500 clinic visits, perform 70 surgeries and admit 300 people for electroencephalography (EEG) studies for epilepsy diagnosis annually. Based on each patient’s individual needs, we offer a wide variety of treatments:
- Minimally invasive laser ablation
- Responsive neurostimulation (RNS)
- Deep brain stimulation
- Vagal nerve stimulation
- Resective brain surgery
Thalamic neurostimulation with the RNS device is our newest procedure. Thalamic neurostimulation directly affects the thalamus, a structure that connects to broad areas of the cerebral cortex, offering the possibility of affecting seizures throughout the brain.
“By using thalamic neurostimulation, we’re trying to hedge our bets and cover a broader territory with brain stimulation,” Poolos says.
Leading advanced investigations
Though several epilepsy medications and surgical therapies exist, there is room for improvement. And the future of research is bright, Poolos says.
- Engineered neurotransmitter cells: As an alternative to resective brain surgery, our Center is evaluating a clinical trial that will inject engineered cells that secrete the neurotransmitter GABA to see if it will inhibit brain activity that prompts seizures. Results of this type of neural transplant look promising.
- Tau protein expression: The protein tau is typically associated with Alzheimer’s disease, but research shows that genetically deleting it has a powerful anti-seizure effect. Our investigators are testing in an animal model the use of the CRISPR gene editing technique to remove tau from neurons located in the areas of the brain where a patient’s seizures start. If successful, this technique would let providers better target their seizure prevention efforts.
- EEG techniques: Our investigators are studying advanced EEG techniques with the ultimate goals of understanding mechanisms and identifying biomarkers of disease.
- Imaging and outcome prediction: Our investigators are engaged in developing methods to better predict seizure outcomes after surgery, including the likelihood of seizure freedom and of cognitive decline. A greater understanding of which patients are likely to be seizure-free will allow better counseling for patients, particularly when risking cognitive side effects.
- Cognitive decline prevention: Our investigators are studying how minimally invasive laser procedures can protect patients against cognitive decline post-surgery.
Collaborating closely to improve care
Our neurological surgery and neurology teams begin their care delivery partnerships with the patient’s first in-person or telehealth visit, Poolos says. The collaboration continues from mapping the patient’s seizures with EEG monitoring through analyzing any imaging and nuclear medicine studies.
Our neurological surgeons, neurologists, neuropsychologists, radiologists and nurse practitioners convene twice weekly to discuss each patient’s case. Together, 10 to 15 people review the patient’s history, epilepsy diagnosis, medication history, EEG monitoring and MRI imaging.
“By being in the same space, we bring everyone’s best ideas together. It’s a very collaborative environment,” Poolos says. “When you have that many people all thinking about a patient’s situation and how we’re going to devise their best treatment path — that’s a very powerful approach.”
Working so closely together also fosters one of UW Medicine’s greatest strengths: clear provider-patient communication.
“We allow our clinicians enough time to sit down and talk to people. Our patients consistently thank us for listening to them and explaining the different treatments,” Poolos says. “I feel like we’re providing care the right way.”
UW Disability Staff and Faculty Association (DSFA)
Good morning,
UW has a new employee affinity group—the UW Disability Staff and Faculty Association (DSFA). Over the last year, this group, which already includes strong representation from both faculty and staff, has been working to build momentum and I am thrilled to serve as their executive sponsor.
Disability is an important part of diversity and our last campus climate assessment indicated that those who identify as having a disability often feel isolated in the workplace. UW’s longstanding employee affinity groups serve as a powerful connector for the communities they welcome and represent. I am confident DSFA will do the same.
I hope you will build awareness through your own leadership communications and diversity efforts. Here is a template to aid in that effort:
UW Disability Staff & Faculty Association (DSFA)
The UW Disability Staff & Faculty Association welcomes anyone who self-identifies as disabled, D/deaf, chronically ill, Mad, neurodivergent, or is an ally to the disability community. Learn more about the supportive environment they are building that honors disability as an important part of diversity.
DSFA joins UW’s longstanding employee affinity groups that are always open and welcoming members and allies:
Asian & Pacific Islander American Association
Black Association
Gay, Lesbian, Bisexual, Transgender, Queer Association
Latinx Association
Native Association
The Office of Minority Affairs & Diversity and UW Human Resources partner on sponsoring UW’s employee affinity groups.
An Innovative Approach to Dementia and Memory Care

Alzheimer’s disease can be a devastating diagnosis. This progressive neurodegenerative condition affects a person’s cognitive abilities, memories and independence in the later stages. In the United States, approximately 6.7 million people are currently affected, and the Alzheimer’s Association expects that number to nearly double to 12.7 million by 2050.
But patients who receive an Alzheimer’s diagnosis don’t need to resign themselves to an inevitable mental decline. New clinical and research advances can change how people live and function with this condition. And UW Medicine is at the forefront of Alzheimer’s and dementia care through the Memory and Brain Wellness Center at Harborview Medical Center.
“We are dedicated to bringing together the clinical research and comprehensive clinical activity to improve memory loss,” says Thomas Grabowski, MD, neurologist and Memory and Brain Wellness Center medical director. “We work hard to combat the stigma of this disease. And we work hard to give people a reason to seek early and accurate diagnosis rather than choosing not to think about it.”
A nationally unique program
The center includes a highly interdisciplinary program that combines the expertise of neurologists, psychiatrists, geriatricians, neuropsychologists and social workers. Together, they provide evaluation and care to people who have experienced memory or cognitive difficulties for at least six months with no prior explanation.
This forward-thinking team takes a two-pronged approach to memory care, Grabowski says. First, they concentrate on strengthening those capabilities patients still have. Second, they foster a dementia-friendly community designed to help patients live well and to their full potential.
To fulfill these two goals, the team created the Memory Hub.
A vibrant, engaging space
Located on the Frye Art Museum campus, the Memory Hub is a philanthropically funded dementia-specific community center that supports individuals with memory loss and their loved ones.
“The Memory Hub grew out of our efforts to build a family and community education program into the Memory and Brain Wellness Center,” Grabowski says. “We aligned with the Frye Art Museum, which had several ongoing arts engagement programs for adults with dementia. We brought together five mission-aligned nonprofits to develop support programming and provide a positive therapeutic program for people with mild memory loss.”
The Memory Hub is an inviting space with classrooms, a lecture hall and a resource library. And its sky-lit atrium is decorated with artwork produced by people with memory loss. Maude’s Garden, named in memory of a community member, offers dementia-friendly landscaping with well-defined pathways. Visitors can also stop in to explore the garden and socialize in a relaxing environment.
Caregivers can also find support and a community of their own through the Memory Hub. They can explore Maude’s Garden with their loved ones during the Garden Discovery program and learn about its therapeutic benefits. They can also meet with Alzheimer’s Association social workers for education about how to best care for their loved one.
Programs for better well-being
In addition to creating a welcoming, memory-friendly community, the center also operates several programs to enhance patient experiences, improve clinical care and advance potential treatment options, Grabowski says.
Some of these programs include:
- Memory Loss: A Guide to Next Steps: During this 90-minute program, newly diagnosed patients and their families talk with dementia experts and peer mentors about strategies to live well with cognitive decline. They also receive a resource handbook called Living with Memory Loss.
- ADAPT: Patients referred from the Memory and Brain Wellness Center clinic can enroll in a two-week mind-and-body wellness program that strengthens their capabilities unaffected by dementia. With a partner — typically a friend or loved one — they commit to 24 hours of program participation. In those sessions, patients learn strategies to manage anxiety and master memory aids.
- Project ECHO® Dementia: This online learning model for clinicians gives front-line dementia providers in Washington state an opportunity to consult with and learn from an interdisciplinary panel of experts. These virtual conferences include topic-specific presentations, such as speech and language, seizure, disease-modifying medications and case-based learning.
- Alzheimer’s Disease Research Center: Through this federally funded center, all patients with a dementia diagnosis can participate in either clinical trials or other observational efforts. The center also maintains brain tissue, blood and spinal fluid samples researchers can use in investigations throughout UW Medicine.
Benefits
Overall, Grabowski says, the center’s biggest effect has been on how patients perceive their future lives after receiving a dementia diagnosis.
“We’re giving people tools to lean into mild cognitive impairment, mild or mid-stage Alzheimer’s or early dementia,” Grabowski says. “When you hear that confirmed diagnosis, it’s often a life-changing moment. Our work empowers people as they move forward and live with this condition.”
In essence, he says, patients feel like they have the support they need to continue living a healthy, productive life. They are less likely to embrace the narrative of loss traditionally surrounding dementia. By continuing to foster a sense of well-being and hope, the Memory and Brain Wellness Center and the Memory Hub will remain vital parts of memory care.
“As we move into an era with more therapeutic options for Alzheimer’s disease, the need for a place like the Memory Hub is only going to increase,” he says. “If we’re successful in delaying Alzheimer’s and slowing the process down before people develop severe symptoms, people will spend more time only mildly impaired. That means we won’t have to deal with more advanced dementia as much — and that’s a good thing.”
UW Medicine Neurology on Pace to Transform Rural Health

For Thabele (Bay) Leslie-Mazwi, MD, the UW Medicine Department of Neurology is more than the only group of academic medicine specialists providing neurological services to Washington state and the Pacific Northwest. It’s a team of providers uniquely positioned to transform care for the thousands of people living in the area’s most remote locations.
“For rural populations in America, the picture of healthcare is not a good one. They have higher mortality and chronic disease rates than urban groups, and their life expectancy is lower,” says Leslie-Mazwi, Chair of the Neurology Department. “They suffer from issues of health equity on an immense scale because they simply don’t have enough access to care.”
Boosting access is where the Neurology Department can make the biggest impact, he says. By using their expertise in clinical care, research and education, providers can change how patients receive life-altering or life-saving care.
Reaching more patients
Truly moving the needle on neurological care means investing in methods that can deliver timely services to more patients. The question, Leslie-Mazwi says, has been how to do it.
“Figuring out how to provide access to specialty care to all these people in all these places is the challenge,” he says. “It boils down to dividing our efforts into two categories: bringing the patient to us and taking care to the patient.”
- Transporting patients: Through UW Medicine’s partnership with Airlift Northwest, providers can transport patients experiencing cerebrovascular, neurotrauma and neurocritical care emergencies directly to one of three landing pads on top of the Harborview Medical Center. This 24/7 service, including five helicopters and four jets stationed across the region, transported almost 500 patients needing emergent or urgent neurological care in 2022, among the thousands of patients transported to UW Medicine in Seattle. “Some of these patients are flying for six hours in one of our fixed-wings to reach our services,” says Leslie-Mazwi.
- Taking care to patients: Fortunately, not every case is an emergency. In these instances, providers use three strategies to meet patients where they live.
- Travel: Providers from UW Medicine Neurology travel to remote communities — from the Olympic Peninsula to Alaska to Idaho — to meet patients where they are, in concentrated clinics held in partnership with health centers in these locations.
- Telehealth: Many providers take themselves to the patient’s location virtually. Through video consultation and telestroke services using telemedicine, they can connect with the patient directly or with the referring provider.
- ProjectECHO: Instead of working directly with patients, UW Medicine providers meet virtually with physicians in rural areas to discuss cases. Currently, 68 remote sites connect for provider-to-provider video consultation programs covering dementia, multiple sclerosis, autism and other conditions. It’s an opportunity for rural physicians to ask patient-centered questions, Leslie-Mazwi says. “When these clinicians share their cases, we have the chance to enhance the expertise and knowledge within the provider community. We’re not providing direct patient care, but we’re informing clinicians about what to do in these situations, in a collaborative and inclusive learning environment. This is a data-driven method to efficiently enhance patient outcomes.”
Expanding neurological research
Part of the health inequity rural populations experience stems from their lack of opportunities to participate in research. Large urban hospitals typically conduct clinical studies, including those focused on neurological conditions. As a result, patients in remote locations may not have access to new medications or therapy options under investigation.
UW Medicine neurologists hope to open this door for more people in remote locations.
“One of the things we are working on doing better — and doing more of — is including rural populations directly in our research,” Leslie-Mazwi says. “We need to do a better job of understanding what these communities face. Telehealth is a crucial part of this effort.”
Training the next generation of physicians
The department is also dedicated to changing the future face of neurological care. That effort means giving residents and fellows hands-on experience in providing services in rural locations.
“We consider our entire land region an immense classroom for our trainees,” Leslie-Mazwi says. “We have multiple sites where our trainees can interact with and learn from more than 200 courtesy clinical neurology faculty, who provide extraordinary neurological care in a range of environments.”
These faculty are invited to participate in department activities, like Grand Rounds, and host UW Medicine trainees in their local centers.
Taking on additional challenges
Increasing rural access to care isn’t a challenge UW Medicine neurologists tackle for the WWAMI alone, though finding answers to these problems will transform healthcare delivery in the WWAMI region’s rural locations. The ultimate impact has the potential to reach much farther.
“I remind our faculty that the neurological solutions we’re testing, refining and disseminating are solutions that can be applied in most areas of the world, where there are a limited number of neurological experts and large geographies that need care,” Leslie-Mazwi says. “I feel like we’re all part of something bigger than our work at UW Medicine alone. We strive to take on challenges and find solutions that will have an impact globally.”
UW Medicine MS Walk – Sunday, April 23, 2023

A new twist on post-stroke neuropalliative care delivery and goals-of-care discussions
Dr. Nauzley Abedini